Abstract
Background: Hereditarythrombophilias (HT) are a group of inherited diseases that predispose to venous thromboembolism (VTE). It can increase the risk of VTE by 3 to 20-fold compared to general population. HT are common and present in 7% of the population. Testing for HT is routine but knowing when to order the tests and how to interpret the results can be challenging. In the United Kingdom, it is estimated that 30,000 tests are done each year to screen for HT with an annual cost of 15,000,000 Euros. This led the British Committee For Standards in Haematology (BCSH) to release guidelines in 2010 that recommends against testing patients at the time of acute venous thrombosis as it will not influence the initial treatment. In the United States there are no clear guidelines regarding testing for HT. We performed a retrospective study to look at the utilization of HT tests among hospitalized patients. This study attempts to address the clinical utility of these tests and concurrent costs to the health care system.
Methods: This is a retrospective study. We reviewed 2402 patient charts with at least one HT test ordered between 2/2016-1/2018 in St Luke's Health Care System records in Kansas City, MO. The following HT tests were included: Activated protein C resistance, antiphospholipid panel, antithrombin III level, factor V Leiden mutation, factor VIII level, homocysteine level, protein C level, protein S level, and prothrombin 20210 mutation. Only patients who had testing done during hospitalization were included. Positive actionable tests were analyzed to determine the clinical benefit of ordering the tests. A positive actionable test was defined as a positive test that changed the anticoagulation intensity, type or duration. Patients with history of previous thromboembolic disease, ongoing medical condition requiring life-long anticoagulation (such as atrial fibrillation), or unprovoked thromboembolic disease were considered non actionable. We also documented the total number of positive tests, ordering providers, and total cost related to ordering these tests (total cost of tests+ cost of hematology consult after an abnormal test).
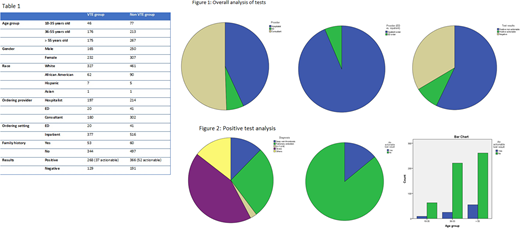
Results: A total of 2402 patients were reviewed. 954 patients were included with a mean age of 54 years. 397 (41.6%) were ordered for venous thromboembolism (VTE) (Deep vein thrombosis, pulmonary embolism or both). Among the included patients, 634 had at least one positive test (Table-1). Only 89 positive tests were actionable (14% of the positive tests and 9.3% of the total ordered tests). There was a statistically significant association between increasing age and having both a positive test result (P-value 0.006), and an actionable test (P-value 0.046). The chance of having actionable tests was more if the test was done in an inpatient setting rather that in the emergency room (OR 0.361, CI 95% (0.177-0.737)). The total cost of ordering these tests was estimated to be $551,218.1 and the cost of subsequent hematology consults was $15,367 leading to total cost of $566,585 during our study period.
Conclusion: Inpatient testing for thrombophilia is associated with increased health care cost and did not change management in many situations. The decision of ordering these tests should be based on a clinical risk assessment.
No relevant conflicts of interest to declare.
Author notes
Asterisk with author names denotes non-ASH members.